In recent years, a model of innovation has emerged in the developing world that seeks to solve problems by making a virtue out of necessity. Low-cost technologies and designs that succeed in their countries of origin are exported to the developed world thanks to their efficiency and simplicity.
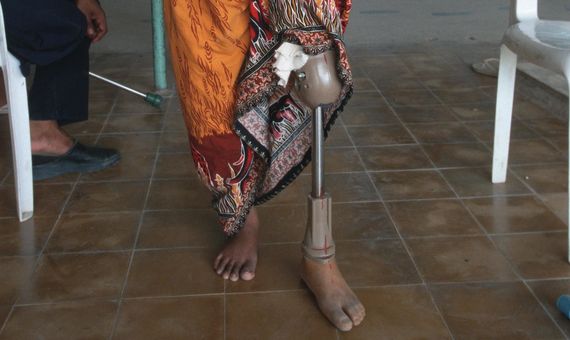
In the early 1990s, Dr. Therdchai Jivacate began working on a revolutionary idea: providing prostheses to citizens of Thailand at reasonable prices. The key to this story probably lies in the concept of “reasonable”. Is it reasonable to ask for up to $20,000 for a prosthetic leg in a country in which people earn $2 a day? Therdchai Jivacate thought it was reasonable for a Thai farmer to pay $30 for a prosthesis, and thanks to his innovative spirit he converted a smart idea into reality. Starting from recycled plastic yogurt containers, his foundation molds prosthetic legs and feet that make life easier for thousands of people.
Reverse innovation: when the need intensifies
The solution is cheap, but it is not done on the cheap. “As counterintuitive as it may seem, the quality demanded by poor people tends to be higher than the quality demanded by the rich,” says Vijay Govindarajan, one of the men who knows best about investing in innovation in developing countries. The inhabitants of the rural areas of Thailand do not need artificial limbs to walk on the sidewalks of a large western city, but rather to get into the rice fields, transport goods by bicycle or climb trees. This is why prostheses should be more durable, stronger and more manageable.
“It’s about pushing the performance paradigm and offering more for less,” sums up Govindarajan, creator of the term “reverse innovation” which defines these bursts of ingenuity that arise where the need intensifies, in Southeast Asian countries, in Africa or Latin America, and whose achievements can be exported to the first world. Today, while it costs many people in developed countries a fortune to pay for prostheses, the victims of land mines in Laos, Myanmar, Malaysia and Thailand have solutions that fit both their legs and their pocketbooks.
Govindarajan began developing this concept when he discovered that many of the sophisticated Western inventions did not reach developing countries due to their high cost and complex operation. In the years in which he led the innovation department of General Electric, the U.S. giant developed a device that performs electrocardiograms and only costs $500, compared to the $10,000 price tag of those found in hospitals in Europe or the U.S. Moreover, its simple operation does not require the use of a specialized technician who also takes care of maintenance. It was developed with the needs of India or Africa in mind but it has been sold by the thousands in 125 countries.
Now, it is the innovators of the poorest regions of the world who are designing their own technological solutions for a pittance, perfectly tailored to their needs and exportable to the developed world thanks to their efficiency. “Because per-capita incomes are so low in the developing world, conditions are ripe for innovations that offer decent quality at an ultralow price—that is, a 50% solution at a 5% price. At first, the 50% solution is unattractive in the rich world, but eventually, performance rises to the point that it is attractive in the rich world,” write Govindarajan and Chris Trimble in their blog.
Healthcare technology as the epicenter of innovation
Examples are beginning to sprout like mushrooms after the rain, such as telemedicine systems developed in Africa that are now being studied in the U.S. for their efficiency and cost-savings. In India, diapers have been developed with a simple chip that can diagnose life-threatening infections when it comes into contact with the baby’s feces. In the past decade, Argentinian car mechanic Jorge Odón invented an inflatable device to assist in difficult vaginal births, replacing the use of harmful forceps. The system, which is supported by the World Health Organization, was purchased by the Becton Dickinson company for development and is now in clinical trials.

Reverse innovation, which is born among the poor and dazzles the rich, has begun to find its place in the world thanks to a talent for making a virtue out of a lack of resources. And one of the key objectives is, obviously, health care: it is better to invent a new method than to adapt one brought in from outside.
“In general, efforts to design new technologies in low-resource places have been more successful than attempts to adapt existing technologies by eliminating more costly or complex features,” bioengineer Rebecca Richards-Kortum and her collaborators wrote in the journal Science. These researchers from Rice University in Houston concluded, after spending time in Africa studying their healthcare systems, that the best approach is to encourage innovation in these countries in order to provide solutions to their problems.
Going a little beyond the classic “teach to fish rather than give a fish,” Richards-Kortum and her collaborator Maria Oden designed a program that provides tools and knowledge for innovation in health in low-resource settings where the design enters into conflict with shortages of electricity and drinking water, scarcity of funds, lack of supplies, absence of trained users and insufficient policy innovation.
For example, thanks to a breathing apparatus for the resuscitation of newborns that operates manually, is self-inflating and does not need electricity, infant mortality in Tanzania has been reduced by 47%. In collaboration with the University of Malawi, a device has been developed to treat respiratory problems in infants using fish aquarium pumps. The system, which in Malawi has boosted the survival rate of these babies from 24% to 65%, is already used in more than 30 countries, and provides the same care as therapies that cost up to $6,000 in the U.S., for 15 times less.

Less expensive but no less efficient: Richards-Kortum and her collaborators say that after a year of clinical evaluation of five machines installed at a hospital in Malawi, not one of them has failed. Normally, in these countries 40% of the breathing devices break down because they are designed to work with stable electrical current flows and not with the unpredictable supply peaks that occur in some parts of Africa. From the Rice 360° Institute for Global Health and in collaboration with local healthcare centers, Richards-Kortum’s team has also designed a device for diagnosing jaundice in infants, and a syringe pump for intravenous medications, all from inexpensive parts and materials available in developing countries.
Improve sanitation and make diagnostic tests cheaper
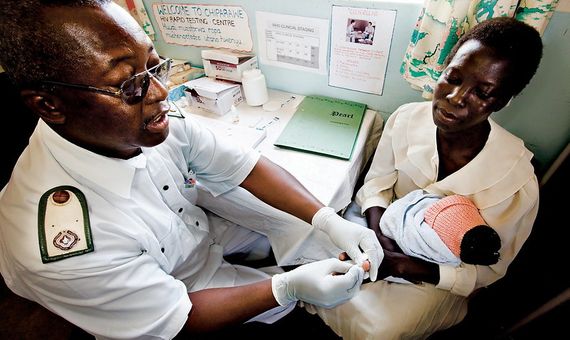
Africa has also begun to develop devices to detect the presence of HIV that meet all WHO recommendations: inexpensive (less than five dollars), user friendly (requiring hardly any prior training), fast and robust (results in less than an hour, no special temperature requirements for transport or storage), and that work without the need to connect to the electric grid.
These initiatives are reminiscent of many of the projects that the Bill and Melinda Gates Foundation is funding for a new generation of cheap, unbreakable and sensitive condoms or to efficiently dispose of organic waste of human origin in populations without sanitation or sewage systems. But it’s not enough: “Alternative approaches are needed to design technologies intended to operate in areas without resources for consumption,” say these bioengineers.
The COVID-19 pandemic has also provided an opportunity for the growth of new reverse innovation initiatives. The state of Massachusetts imported the contact tracing system for infected persons previously used in Africa against diseases such as Ebola, which uses an extensive network of human operators. Rapid response teams have also been created drawing on the experience of developing countries where infectious outbreaks are more frequent. Some developing countries have worked on low-cost respirators and simple, inexpensive testing systems. The most attractive point of these emerging technologies is that they move in the opposite direction to the usual, and they can help make life easier for people not only in poor countries but around the world thanks to the ingenuity that arises when all else fails.
According to Greg Martin, editor of the public health journal Globalization and Health, which since 2012 had dedicated a series to reviewing developments in the field, “these studies illustrate an impetus and a bubbly enthusiasm (both individually and nationally) for pushing global health beyond the narrow limits of traditional thinking. We are aware that there is a large global movement destined to activate the real potential of the low- and middle-income countries to contribute to the challenges of health systems everywhere. We have to learn, share and critique emerging results to promote two-way learning and make rapid progress towards a truly global flow of innovation.”
Comments on this publication