An engineering look at the human body sees the blood as a viscous liquid, which attends to the mechanics of fluids; it observes the bones as if they were the beams and pillars of a building; it identifies the nerves—conductors of electrical impulses—with the complex wiring of a house; it sees in the neural network of the brain the printed circuit of a computer. And just as civil engineering can calculate how a bridge will behave before building it, biomedical engineering predicts how the circulatory system will respond, a very useful forecast to successfully solve some of the most complex medical problems, such as the evolution of an aneurysm, the outcome of open heart surgery or the steps to follow in the event of a stroke.
“It’s possible to model the circulatory system thanks to the advancement of calculation theories and the development of powerful computers. Therefore, its behaviour can be simulated, which will help cardiologists to make more accurate decisions,” says Fermín Navarrina, professor and doctor in engineering at the Superior Technical School of Roads, Canals and Ports of the University of A Coruña (Spain).
Although the personalized simulation of a patient’s blood flow is still in its early stages, it is already useful in multiple scenarios. For example, it allows doctors to know how a vascular implant will behave or the places that are most likely to generate thrombi after heart bypass surgery. Furthermore, it can guide a surgeon, advising them on the best solution to a complex cardiac operation.
Simulation of blood flow
The first surgical intervention in the world to use computerized blood flow simulation took place in 2015, thanks to the calculations of Alberto Figueroa, professor of Biomedical Engineering and Cardiovascular Surgery at the University of Michigan (USA). Since then, his team has participated in dozens of similar experimental operations. “The most common operations in which we work are on patients who were born with a single ventricle, who underwent emergency surgery at the time. What usually happens is that at age 15-20 they begin to once again show symptoms of their congenital problem. So what we do in the operating room is a correction of that original surgery, because back then there was neither the knowledge, nor the technology, nor the technique to plan that operation in the most optimal way,” Figueroa explains to OpenMind.
In order to make simulations of a person’s circulatory system, prior data collection is essential. “The data we need is about the patient’s anatomy and hemodynamics. The anatomy is obtained with a CT scan (Computerized Axial Tomography) or with an MRI scan; these essentially provide something very similar, that is, a three-dimensional picture of the person’s interior. Regarding hemodynamics, we need information about blood velocity, given by the MRI, and blood pressure, which is achieved with the introduction of a catheter into the patient,” says Figueroa.
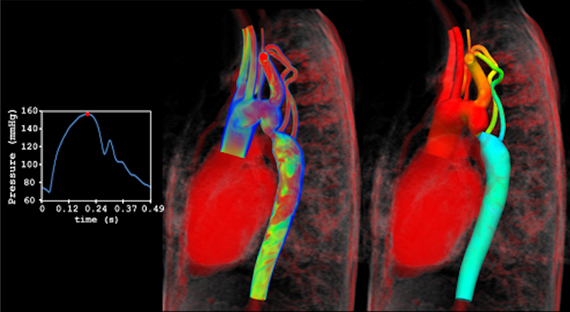
After obtaining these numbers, the next step, the most complex, is to develop a computer model that behaves just like the circulatory system of the patient. Once achieved, the virtual planning of the operation begins. “The cardiac surgeon who is going to operate is the one who tells us the different alternatives which he has thought about, and we test them in our model to determine which behaves better from the hemodynamic point of view,” says Figueroa. However, he insists: “All this is still an experimental process.”
Figueroa is developing open-source software called CRIMSOM (Cardiovascular Integrated Modelling and Simulation) in an attempt to disseminate knowledge and have his studies used by as many researchers as possible. “We want to make it public by the end of 2018,” he says. The ultimate goal is to get surgeons to perform virtual surgical operations in order to choose the best possible option before carrying out the actual operation.
Models of the heart
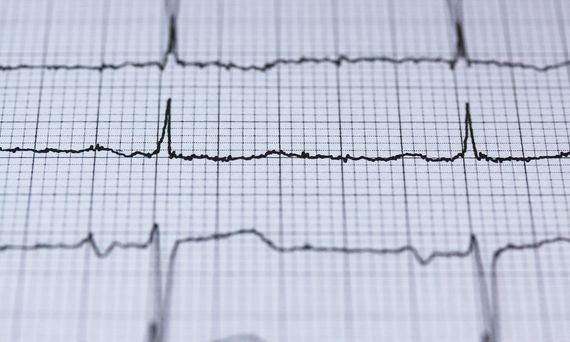
The development of a computer application that specifically simulates a patient’s heart is a challenge that Navarrina’s work team hopes to overcome. “We have been working for almost 30 years on solving problems that are called electrokinetics, that is, electricity in motion. “One of the research projects that we are launching will try to take advantage of this knowledge,” informs the professor. “The heart works from electrical impulses that can be recorded on an electrocardiogram. Although we are still at a very early stage, the final goal of our project would be to find out what areas of a diseased heart are damaged from its electrocardiogram, thanks to the development of behavioural models of that organ,” says Navarrina.
Figueroa is clear that the future of medicine lies with the simulation of the behaviour of the human body before making many medical decisions: “I don’t have any doubt that in 50, 100, 150 years…they will look back to how we do things now with a little horror—similar to how we look at the Middle Ages, when they tried to heal the patient with bloodletting. In part, because we are still developing all these tools, but also because there is still a big disconnect between the way engineering and medicine deal with problems.” Navarrina concludes: “We are standing before an infinite field that has scarcely begun.”
Comments on this publication