A century ago, the Spanish flu, described as “the greatest medical holocaust in history,” claimed between 40 and 100 million lives. Although this sentence is not entirely accurate— neither was the flu Spanish, nor was it really that virus that killed most of the victims—it is still the worst flu pandemic in humanity, responsible for more deaths than the world war with which it coincided. But the crucial question is: do we know enough today to prevent history from repeating itself?
Nowadays we know that the Spanish flu was not like any other, but the first to suspect this was a doctor from the remote county of Haskell, Kansas. In January 1918, Loring Miner observed that a more virulent flu than normal was taking down a good portion of the inhabitants of the county, not children, the elderly and the chronically ill—the usual victims—but rather the young and the strong. In some patients, the disease was aggravated by pneumonia. And then the deaths began.

Miner, who is said to have been a rural doctor of great culture and scientific spirit, alerted the US Public Health Service, but by the time his note was published in April in the journal Public Health Reports, the disease was already receding in Haskell. However, for the rest of the world the worst was just beginning. On March 4, the first case of flu was recorded in Camp Funston (now Fort Riley), the military barracks for the Haskell recruits, some 480 kilometres from the county. In just three weeks, the quantity of infected victims numbered in the thousands.
From the Arctic to the South Pacific
Many of those soldiers were destined for Europe to fight in the First World War. In a few months, the disease had colonized practically the entire planet, from the Arctic to the South Pacific. Of the 500 million affected, most of the deaths occurred in the second wave in the autumn of 1918, although the powers involved in the war silenced the epidemic due to the information censorship imposed by the war.
Only in neutral Spain did the media spread the news about the so-called “three-day flu,” which affected King Alfonso XIII himself. This is how the 1918 pandemic came to be known as the Spanish flu.
Although today it is recognized that the disease did not arise in Spain, the debate about its true origin has not yet been settled. The data from Haskell led writer and historian John M. Barry, author of The Great Influenza: The Epic Story of the Deadliest Plague in History (Viking Books, 2004), to argue that the virus was born in Kansas, but it is still considered an unresolved mystery. “It’s not nailed at all,” says Barry to OpenMind. “Latest molecular biology findings undermine but do not quite eliminate that Haskell hypothesis. It now looks like the virus may have been around in 1917, possibly even earlier.” The most plausible current theories place the source of the virus in China or France.
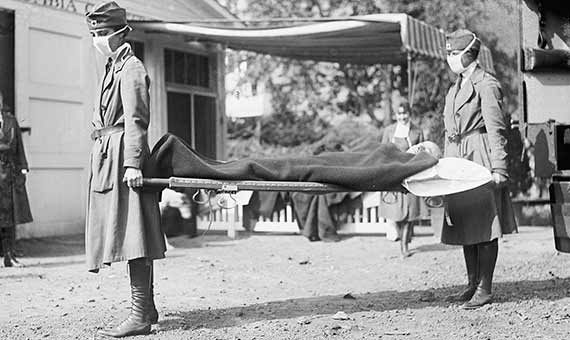
Regardless of its geographical cradle, for a century researchers have tried to unravel what made the virus such a powerful exterminator. As noted by Miner, the Spanish flu showed an unusual lethality pattern, predominating in healthy people of between 20 and 40 years old, with the peak of mortality at age 28. The reports of the time were already noting that the majority of the deaths were not directly due to the flu, but to bacterial pneumonia contracted in a secondary way.
Reconstruction of the virus
In 2005, the recovery of lung tissue from a victim buried in the icy soil of Alaska, along with some preserved samples of US soldiers, allowed the sequencing of the genome and even the reconstruction of the virus under tight security measures at the US Center for Disease Control. Experiments with the recreated virus confirmed its virulence: in infected mice it reproduced itself 39,000 times more than a normal flu. Studies with monkeys also revealed that it tended to trigger what is known as a cytokine storm, a complication that appears because of an exaggerated immune response, which could explain the mortality rates in young people with a more robust immune system.
From the genetic sequence, in 2007 a team of researchers led by Jonathan A. McCullers, of the St. Jude Children’s Research Hospital in Memphis, managed to identify one of the culprits of the lethality of the virus: a particular form of a viral protein called PB1-F2 that aggravated the symptoms of influenza and the secondary bacterial pneumonia. However, McCullers points out to OpenMind that this is probably only “a part of the story” and that the aggressiveness of that virus “is still an open question.” In fact, the influence of other molecular factors on the virulence of the Spanish flu has been demonstrated.

“We have learned a great deal about this virus,” says McCullers. But in addition to the pathogenic mechanisms, there are unanswered questions: whether it jumped to humans from birds or other mammals; if genetics made some people more sensitive than others; or to what extent previous exposure to other viruses in the flu could determine the course of the disease, to improve or worsen it. However, the most intriguing question is: could it be repeated?
Experts often warn that the question is not if it will be repeated, but when. In 2009, the first influenza pandemic of the 21st century, caused by a virus of the same type as that of 1918, caused between 150,000 and half a million deaths. However, the improvement in living standards, vaccines and antibiotics against secondary infections today offer a more potent arsenal against the disease than 100 years ago. “My own opinion is that an event similar to what happened in 1918 is very unlikely,” says Dennis Shanks, director of the Australian Army’s Malaria Institute, tells OpenMind.
However, McCullers points out that the risk could lurk in certain aggressive flus that currently circulate in species such as birds. “Were they able to spread easily between humans, we could see a disaster of a similar magnitude,” the expert fears. “We are now truly a global society, and such a virus could circle the world in a matter of days or weeks.”
Javier Yanes
Comments on this publication