Pandemics are the disasters that have destroyed the most human lives, even changing the course of history. Even recent viruses with an immediate global impact less dramatic than that of SARS-CoV-2, which causes COVID-19, such as HIV, Ebola, epidemic influenzas, SARS or MERS, should already have prepared us to respond to new threats in the future. However, despite the incredible progress of science, it is curious that our best weapons so far to respond to the current pandemic have been so primitive that some have even existed since biblical times: quarantine, isolation, social distancing, hygiene, masks… But just as antibiotics transformed our fight against bacteria, will we find a breakthrough that will give us the ultimate advantage in our war against viruses?
A common question one might ask is why we don’t have the equivalent of antibiotics against viruses, that is, drugs capable of controlling them completely. It comes down to bacteria and viruses being very different entities. The former are generally free-living organisms whose evolutionary path separated from our own in very ancient times; as a result, their cells are remarkably different from ours, allowing us to find compounds that can interfere with their metabolic mechanisms without affecting humans. This is known as selective toxicity.
The discovery of antivirals
The case of viruses is different. Firstly, they are all intracellular parasites that need to use the machinery of the cells they colonise. A virus outside its host is an aggregate of inert organic matter that has no metabolism to interfere with, and when it infects us it is already part of us, so it is more complicated to attack it without battling our own organism. As researchers Christine Carson and Rachel Roper wrote in The Conversation, “this makes it hard to kill viruses without killing our own cells in the process.” “Killing viruses is easy. Keeping host cells alive while you do it is the hard part,” the two experts note.

An additional difficulty is that viruses are enormously diverse. They use a wide variety of cell receptors to invade many different types of cells and thus there is no common mechanism of infection that can be acted upon. This is why the antibiotics available today number in the hundreds, with possibly more than 150 in pre-clinical development, while the number of antivirals has only begun to rise in recent decades; in 1990 they were down to just five, while today they number around 90.
The strategies for the discovery of antivirals are numerous, as are the targets to which they are directed, from inhibiting the binding of the virus to the cell to preventing the formation of new viral particles, to blocking the processing of their genetic material or their proteins. In some cases these drugs are specifically designed to target specific virus components, which is not only a long and laborious process, but also restricts their usefulness to a single pathogen or several closely related ones.
But even when antivirals seek to attack a wider group of viruses with similar mechanisms, their usefulness is often limited. Remdesivir, an experimental drug that is highly topical because of its proven ability to reduce the recovery time of patients battling COVID-19, is billed as a broad-spectrum antiviral because its molecular structure as an analogue of an RNA component suggested it would be an inhibitor of viruses that use this class of genetic material. However, it failed against hepatitis C, the virus for which it was created, and has also been shown to be ineffective against Ebola and Marburg. Most of the drugs available today are only effective against a few viruses, mainly HIV, hepatitis, influenza, herpes, varicella-zoster and cytomegalovirus, and there seems to be no clear prospect of an imminent revolution in the procurement of new antivirals.
Vaccines
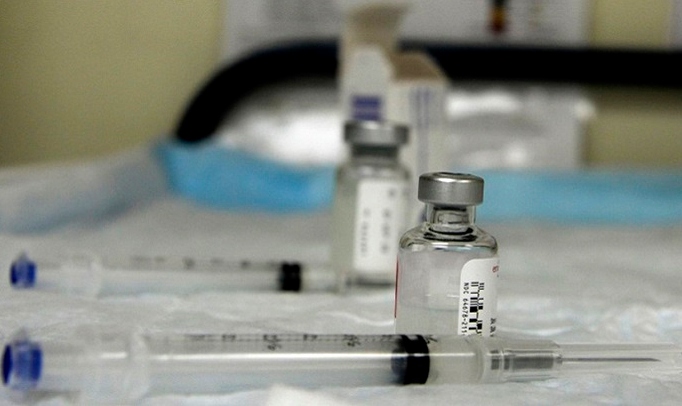
More optimism, although still cautious, exists in the field of vaccines. Traditional methods are based on the attenuation or inactivation of the virus, techniques that have proven effective but require starting from scratch for each emerging pathogen. In contrast, a novel approach focuses on building standardised platforms that can be quickly and easily adapted to any new virus by replacing only a few parts. This is how RNA or DNA vaccines work, in which researchers need only know the genetic sequence of the virus to synthesise it and introduce it into the platform. Inovio Pharmaceuticals stated that, after the SARS-CoV-2 genome was sequenced, it took just three hours to have a prototype vaccine designed on paper. Although this claim has been questioned, the truth is that these technologies have the potential to accelerate the development of vaccines as long as they prove their effectiveness, since there are no approved vaccines on the market yet.
However, the future of the fight against viruses does not have to focus exclusively on attacking the pathogen. Every viral infection consists of two parts, the attack of the virus and the defence of the organism. And while the first component is always an unknown, subject to an infinite number of variables with every new virus that emerges in nature, the repertoire of responses by the organism is more limited and to some extent better understood, so acting on it to regulate it at will could offer a truly broad-spectrum strategy against any viral threat.
How do we survive infections?
This is what immunologist Janelle Ayres of the Salk Institute explained in an editorial published in Science last April: “Instead of asking ‘how do we fight infections?’ we might start asking ‘how do we survive infections?’” she wrote. The proposal is to apply strategies to tolerate the infection and allow the body to survive until the disease subsides, that is, save the patient, not fight the virus. For the immunologist, “there is no scientific or public health reason for why we have not developed such therapies.” And yet, although this approach could provide weapons even against future as yet unknown pathogens, this has been a traditionally under-exploited field in the war against viruses, because, according to Ayres, “the perspective for combating infectious diseases shared by scientists is incomplete.”

In the same vein, during the COVID-19 pandemic it has become clear that at least a proportion of deaths are related to a harmful overreaction of the patient’s own immune system, something that had already been observed in other viral infections. There is still no conclusive data on what percentage of patients with COVID-19 develop this hyperinflammatory response, known as Cytokine Release Syndrome or, more popularly, cytokine storm. But recent studies have identified differences between the disturbances of the immune response in mild and severe patients, as well as changes related to the progression of the disease, which could aid in finding mechanisms to boost the defences against the virus while avoiding overreactions that are harmful to the body itself. For example, some studies point to a possible treatment through interferons, the natural antivirals that our body manufactures to fight viral infections. Clinical trials are already underway that point to promising results from this strategy against COVID-19.
Ultimately, it doesn’t seem like we are close to finding a magic bullet against viruses. But if something useful has emerged from the current pandemic, it is that it has spurred countless scientists from the most diverse disciplines to propose solutions from fields even far removed from the biomedical sciences. At the University of Michigan, engineer Herek Clack has developed a plasma reactor capable of inactivating viruses in the air, which according to its creators reduces the amount of infectious viruses by more than 99% and could be installed on commercial aircraft. Human ingenuity still has much to contribute beyond quarantines and masks.
Javier Yanes
@yanes68
Comments on this publication